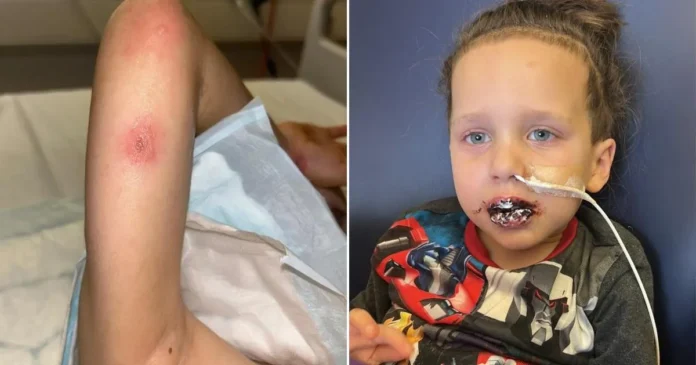
A determined mother repeatedly advocated for her five-year-old son, Mylo, after doctors initially dismissed his severe symptoms as a common childhood illness, sending the family home despite clear signs of distress.
First Episode: Blisters and Swelling in Late 2024
In November 2024, Mylo woke up with blisters on his hands and around his mouth. A doctor initially diagnosed hand, foot, and mouth disease (HFMD), recommending paracetamol, ibuprofen, and plenty of fluids.
The next day, his eyes swelled shut, and the mouth blisters prevented him from drinking. At the hospital, staff admitted him for three nights, suspecting HFMD complicated by gingivostomatitis—a severe mouth infection. He received IV fluids and antiviral drugs, showing improvement before discharge.
However, symptoms returned quickly at home, with swelling around his lips and eyes. Readmitted, a doctor raised concerns about Stevens-Johnson Syndrome (SJS), a rare and serious skin disorder often triggered by infections in children. “Do not Google it,” the doctor warned.
Daily eye exams monitored risks of scarring, corneal damage, or even blindness from inflammation. After five days, the swelling subsided, allowing discharge. The mother stayed strong in front of Mylo but broke down privately from fear.
Recurrence Strikes in December 2025
Thirteen months later, in December 2025, Mylo developed a cough and cold. Five days in, a blister appeared on his lip, followed by another inside his mouth. Despite reassurances that recurrence was unlikely, the parents rushed him to the hospital.
Doctors again suggested HFMD and sent them home. That night, Mylo’s fever spiked, prompting another visit. This time, staff recognized the severity and admitted him.
Tests confirmed chickenpox, likely triggering a recurrence. Blisters and swelling engulfed his lips, eyes, and genitals, preventing him from drinking even through a straw or speaking clearly. Interactions relied on nods and thumbs-up.
Treatment included morphine for pain, a nasal NG tube for nutrition, and constant care to manage drooling. The diagnosis: RIME (Reactive Infectious Mucocutaneous Eruption), a condition mimicking SJS, triggered by infections. Doctors suspected the prior episode was also RIME.
Treatment, Recovery, and Ongoing Concerns
With dead skin tissue building in his mouth and no quick improvement, surgeons considered sedation to remove it. Fortunately, after six days, Mylo began sipping liquids. He returned home still covered in lesions, requiring steroid eye drops until January, sponge cleaning for his lips, and weekly hospital monitoring.
Genetic testing with a pediatric consultant is scheduled for April to check for susceptibility genes. Vitamins now bolster his immune system against future infections.
Mylo has returned to school, football, and play with friends, showing no lasting damage. Yet, uncertainty lingers—any cold could trigger another episode in an active five-year-old.
The mother urges parents to trust their instincts: “No one knows your child better than you.” Her persistence proved vital amid initial dismissals.